Patients Advised to Take More Blood Pressure Pills
Worldwide headlines were released on September 11, 2015, through the general media (newspapers, Internet, radio, and TV), about benefits derived from more aggressively treating high blood pressure (hypertension) with drugs. This news was based on the unpublished SPRINT trial: a randomized clinical trial of over 9,000 Americans, 50 years and older with high blood pressure, and an increased risk for heart and/or kidney disease. Half the participants were given a blood pressure target of 120 mmHg systolic pressure (top number) and the other half were given a target of 140 mmHg. An average of 3 kinds of antihypertensive medications were needed to reach the lower target goal (120 mmHg), whereas, only 2 drugs achieved the higher target (140 mmHg). The new target of 120 mmHg was publicized to reduce the rate of heart attacks, heart failure, and stroke by 30%, and cardiovascular deaths by 25%. (Likely, these figures are relative risk reductions, rather than absolute reductions, which means the perception of benefit is greatly exaggerated.)
This news release was bold, unusual, and improper because no evidence, statistics, or other information necessary to evaluate the clinical worthiness of these findings was simultaneously released. The scientific data required to independently assess the value of the SPRINT study will not be fully available until 2017; however, the practice of medicine has been changed, today, with this news. Drug companies have directly funded many of the people and organizations involved in the SPRINT study, yet no conflicts of interest have been reported that could point to strong financial biases.
One undeniable result of this media campaign to have physicians prescribe more pills is to bring tens of billions of dollars to the pharmaceutical industry. Furthermore, physicians, emergency rooms, and hospitals will experience financial gains from initiating more treatment, and the side effects that always follow. There has been nothing in the news releases about the potential harms of treating to a lower target of 120 mm Hg. Past research has shown that aggressive treatment of blood pressure with medications increases the risk of stroke, heart attacks, and death.
For treating high blood pressure, my fundamental recommendation is for a change in diet…and then, judicious use of medication (usually chlorthalidone) for people with a sustained blood pressure of 160/100 mmHg or greater. My target blood pressure with medication is no lower than 140/90 mmHg.
How I Treat Patients with Elevated Blood Pressure
From the November 2009 McDougall Newsletter
Elevated blood pressure, or hypertension, is associated with serious health problems, such as strokes, heart attacks, and kidney failure. Most people believe the problem with hypertension is that the elevated pressure damages the arteries and the body’s organs. Actually, it is more often the other way around. The rise in blood pressure is a response to a sick body—the blood pressure goes up as a natural and proper adaptation—as an attempt to compensate for a plugged up cardiovascular system. After years of consuming the rich Western diet, the blood vessels develop blockages referred to as atherosclerosis, the artery walls stiffen, and the blood itself becomes viscous. All this change creates a resistance to flow, resulting in a decrease in the ability to deliver nutrients to the tissues. The body responds, as it should, with a rise in blood pressure.
The correct action for the patient to take is to decrease the resistance to flow by eating a healthy diet and exercising. Most people who follow the McDougall diet find their blood pressure decreases within a few days. Based on several collections of results from my clinic, the average reduction of blood pressure is about 14/11 mmHg in seven days, and at the same time medications used for treating hypertension are usually stopped. My customary protocol is to stop all blood pressure-lowering medications the first day of the Program, except for beta-blockers, which I slowly discontinue by cutting the dosage in half every two to three days. Unfortunately, not every patient experiences the reduction in numbers they desire. Despite their best efforts some people may need medications.
These blood-pressure-lowering drugs function by poisoning the body in various ways. “Poison” is the correct word. In chemistry poison means to inhibit a substance or a reaction. Beta-blockers inhibit the action of adrenalin on the heart muscle, calcium channel blockers inhibit the contraction of the blood vessels, ACE inhibitors and angiotensin receptor blockers do just that (inhibit and block) the blood pressure regulating hormones produced by the adrenal glands, and diuretics poison the water and electrolyte conserving functions of the kidneys.
These five major classes of medications are discussed in more detail below.
Take Measurements at Home for Months before Starting Drugs
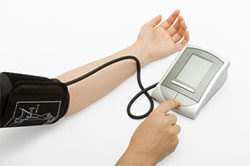 Before starting medications in non-emergency situations, people with concerns about their blood pressure should first, buy a good quality blood pressure cuff (an oscillometric monitor for $50 to $100) and use it to monitor their blood pressure at home.1 I suggest they then record the values several times a week and take these numbers to their private doctor for further discussion.
Before starting medications in non-emergency situations, people with concerns about their blood pressure should first, buy a good quality blood pressure cuff (an oscillometric monitor for $50 to $100) and use it to monitor their blood pressure at home.1 I suggest they then record the values several times a week and take these numbers to their private doctor for further discussion.
A sustained elevation of blood pressure to 160/100 mmHg or greater over months suggests the need for treatment with medication.2 A word of caution: If you do start blood pressure-lowering medications, avoid overly aggressive treatment. In general, reducing blood pressure below 140/90 mmHg with medication is not beneficial and actually will increase the risk of heart attacks, strokes, and death.3,4 A recent review by the well-respected Cochrane Collaboration concluded with: “Treating patients to lower than standard BP targets, ≤140-160/90-100 mmHg, does not reduce mortality or morbidity.”5
Chlorthalidone Is the Drug of Choice
Chlorthalidone is an oral diuretic (a water pill taken by mouth) with a prolonged action of 48 to 72 hours and low toxicity. Diuretics lower blood pressure by reducing fluid volume, which decreases the output of the heart causing the blood pressure to fall. Doctors and patients often believe that all diuretics have similar benefits. This is not the case, and chlorthalidone is the preferred kind of diuretic for most patients.6,7 In 1990, the Multiple Risk Factor Intervention Trial (MRFIT) reported a reduction in nonfatal cardiovascular events when the diuretic treatment was changed to replace hydrochlorothiazide (HCTZ) with chlorthalidone in men at high risk for coronary heart disease.8 Chlorthalidone is also more effective at lowering systolic blood pressure (the top number) than HCTZ. The starting dosage used was 12.5 to 25 mg daily; but the dosage can be increased to 50 to 100 mg daily. All patients receiving chlorthalidone should be checked after one month for evidence of fluid or electrolyte imbalance: namely, low sodium, low chloride, and low potassium (by blood tests). Other periodic laboratory tests should be performed to look for adverse effects from this potent diuretic. For example, blood levels of cholesterol, triglycerides and uric acid can be increased by this medication. Chlorthalidone is inexpensive; a 30-day supply is $4 and a 90-day supply is $10 for 25 or 50 mg tablets at Walmart.
Why I No Longer Routinely Prescribe Beta-blockers
For many years beta-blockers were considered one of the first line therapies for the treatment of hypertension. Current evidence suggests that beta-blockers (like Atenolol) should not be prescribed unless there is some other reason for their use (like atrial fibrillation, heart failure, or myocardial infarction).9 A recent Cochrane Collaboration concluded: “The available evidence does not support the use of beta-blockers as first-line drugs in the treatment of hypertension. This conclusion is based on the relatively weak effect of beta-blockers to reduce stroke and the absence of an effect on coronary heart disease when compared to placebo or no treatment.”10
Examples of commonly prescribed beta-blockers are: acebutolol (Sectral), atenolol (Tenormin), betaxolol (Kerlone), betaxolol (Betoptic, Betoptic S), bisoprolol fumarate (Zebeta), carteolol (Cartrol), carvedilol (Coreg), esmolol (Brevibloc), labetalol (Trandate, Normodyne), metoprolol (Lopressor, Toprol XL), nadolol (Corgard), nebivolol (Bystolic), penbutolol (Levatol), pindolol (Visken), propranolol (Inderal, InnoPran), sotalol (Betapace), and timolol (Blocadren).
I Never Prescribe Calcium Channel Blockers
Calcium channel blockers are also called “calcium antagonists” and “calcium blockers.” They may decrease the heart’s pumping strength and relax the blood vessels, and are commonly used to treat high blood pressure, angina (chest pain), and some arrhythmias (abnormal heart rhythms). However, they increase the risk of dying from heart disease and cancer (especially breast cancer), and the risk of developing open-angle glaucoma, suicide, and bleeding.11-17
Examples of commonly prescribed calcium channel blockers are: amlodipine (Norvasc), clevidipine (Cleviprex), diltiazem (Cardizem), felodipine (Plendil), isradipine (Dynacirc), nifedipine (Adalat, Procardia), nicardipine (Cardene), nimodipine (Nimotop), nisoldipine (Sular), and verapamil (Calan, Isoptin).
I Never Prescribe Angiotensin Receptor Blockers (ARBs)
Angiotensin is a hormone found in the body that causes blood vessels to constrict, resulting in higher blood pressure and extra work on the heart. Angiotensin receptor blockers (ARBs), also called angiotensin II receptor antagonists, prevent angiotensin from binding to its receptor in the walls of the blood vessels. This results in a lower blood pressure. These medications are often prescribed because they are less likely to cause a chronic cough than medications called angiotensin converting enzyme inhibitors (ACE Inhibitors), which also work on the “angiotensin system” to control high blood pressure.
Convincing evidence shows that angiotensin receptor blockers (unlike ACE inhibitors) increase the rates of myocardial infarction (heart attacks) despite their beneficial effects on reducing blood pressure.18
Examples of commonly prescribed angiotensin receptor blockers are: candesartan (Atacand), eprosartan (Tevetan), irbesartan (Avapro), telmisartan (Mycardis), valsartan (Diovan), and losartan (Cozaar).
ACE Inhibitors Are Less Beneficial and More Dangerous Than Advertised
Angiotensin converting enzyme inhibitors (ACE Inhibitors) have been used for decades to treat hypertension and heart disease. Their main selling point is that they are said to be “renal-protective,” meaning they help protect the kidneys from failing, especially for people with already existing kidney disease and/or diabetes. However, their value for protecting the kidneys has been largely refuted.20-23 The ALLHAT data (the largest antihypertensive trial and the second largest lipid-lowering trial) showed that among those patients with diabetes, more patients in the ACE inhibitor (lisinopril) group progressed to end stage kidney failure compared with the chlorthalidone group.23 Acute and chronic kidney failure from the use of these drugs is also reported (and is much more common than most doctors realize).19,23
Examples of commonly prescribed ACE inhibitors are: benzapril (Lotensin), captopril (Capoten), enalapril (Vasotec), fosinopril (Monopril), lisinopril (Prinivil, Zestril), moexipril (Univasc), perindopril (Aceon), quinapril (Accupril), ramipril (Altace), and trandolapril (Mavik).
Medication Benefits Are Oversold
Not surprisingly, pharmaceutical companies make great efforts to advertise the benefits of their products and to cover up the harms. To be more blunt, these companies lie to doctors, patients, medical journals, and the media.24 One common method used is to report unimportant benefits from use of their products, such as lowering the blood pressure, rather than reporting very important end points like staying alive and reducing the risk of a stroke or heart attack.
They also report “relative benefits” rather than “absolute benefits.” For example, the risk of stroke over five years is fifteen cases per thousand for untreated patients and nine cases for those actively treated with medications.25 The relative risk reduction is 15 minus 9 divided by 15 or a 40% reduction. Forty percent sounds like a great benefit. However, figuring more honestly with reports of the absolute benefit are far less impressive. The absolute reduction in stroke from treatment with medication is 15 minus 9 strokes, which equals only 6 strokes prevented after treating a thousand people with medication for five years. In other words, annually, one stroke is prevented by treating one thousand patients. That’s a lot of money spent and side effects suffered for a very low absolute benefit. (Would you trade sexual dysfunction for this one in a thousand possible benefit?)
The bottom line is this: Make all efforts to avoid the need for medications or any other medical services by staying healthy. This means following the McDougall diet, exercising and practicing clean habits.
References:
1) Pickering TG, Miller NH, Ogedegbe G, Krakoff LR, Artinian NT, Goff D. Call to Action on Use and Reimbursement for Home Blood Pressure Monitoring: Executive Summary. A Joint Scientific Statement From the American Heart Association, American Society of Hypertension, and Preventive Cardiovascular Nurses Association. Hypertension. 2008 May 22.
2) Williams B, Poulter NR, Brown MJ, Davis M, McInnes GT, Potter JF, Sever PS, Thom SM; BHS guidelines working party, for the British Hypertension Society. British Hypertension Society guidelines for hypertension management 2004 (BHS-IV): summary. BMJ. 2004 Mar 13;328(7440):634-40. http://www.ncbi.nlm.nih.gov/pmc/articles/PMC381142/?tool=pubmed
3) https://www.drmcdougall.com/misc/2004nl/040700pubp.htm
4) https://www.drmcdougall.com/misc/2006nl/august/fav5.htm
5) Arguedas JA, Perez MI, Wright JM. Treatment blood pressure targets for hypertension. Cochrane Database Syst Rev. 2009 Jul 8;(3):CD004349
6) http://www.medscape.com/viewarticle/479473
7) The Medical Letter, Volume 51 (Issue 1305) February 9, 2009
8) Carter BL, Ernst ME, Cohen JD. Hydrochlorothiazide versus chlorthalidone: evidence supporting their interchangeability. Hypertension. 2004;43:4-9.)
9) Carlberg B, Samuelsson O, Lindholm LH. Atenolol in hypertension: is it a wise choice? Lancet. 2004 Nov 6;364(9446):1684-9.
10) Wiysonge CS, Bradley H, Mayosi BM, Maroney R, Mbewu A, Opie LH, Volmink J. Beta-blockers for Hypertension. Cochrane Database Syst Rev. 2007 Jan 24;(1):CD002003.
11) Psaty BM, Heckbert SR, Koepsell TD, Siscovick DS, Raghunathan TE, Weiss NS, Rosendaal FR, Lemaitre RN, Smith NL, Wahl PW, et al. The risk of myocardial infarction associated with antihypertensive drug therapies. JAMA. 1995 Aug 23-30;274(8):620-5.
12) Beiderbeck-Noll AB, Sturkenboom MC, van der Linden PD, Herings RM, Hofman A, Coebergh JW, Leufkens HG, Stricker BH. Verapamil is associated with an increased risk of cancer in the elderly: the Rotterdam study. Eur J Cancer. 2003 Jan;39(1):98-105.
13) Fitzpatrick AL, Daling JR, Furberg CD, Kronmal RA, Weissfeld JL. Use of calcium channel blockers and breast carcinoma risk in postmenopausal women. Cancer. 1997 Oct 15;80(8):1438-47.
14) Pahor M, Guralnik JM, Ferrucci L, Corti MC, Salive ME, Cerhan JR, Wallace RB, Havlik RJ. Calcium-channel blockade and incidence of cancer in aged populations. Lancet. 1996 Aug 24;348(9026):493-7.
15) Lindberg G, Bingefors K, Ranstam J, Rastam L, Melander A. Use of calcium channel blockers and risk of suicide: ecological findings confirmed in population based cohort study. BMJ. 1998 Mar 7;316(7133):741-5.
16) Pahor M, Guralnik JM, Furberg CD, Carbonin P, Havlik R. Risk of gastrointestinal haemorrhage with calcium antagonists in hypertensive persons over 67 years old. Lancet. 1996 Apr 20;347(9008):1061-5.
17) Müskens RP, de Voogd S, Wolfs RC, Witteman JC, Hofman A, de Jong PT, Stricker BH, Jansonius NM. Systemic antihypertensive medication and incident open-angle glaucoma. Ophthalmology. 2007 Dec;114(12):2221-6.
18) Verma S, Strauss M. Angiotensin receptor blockers and myocardial infarction. These drugs may increase myocardial infarction – and patients may need to be told. BMJ 2004 Nov 27;329:1248-9.
19) Onuigbo MAC. Reno-prevention vs reno-protection: a critical re-appraisal of the evidence-base from the large RAAS blockade trials after ONTARGET—a call for more circumspection. QJM. 2009;102(3):155-167.
20) Suissa S, Hutchinson T, Brophy JM, Kezouh A. ACE-inhibitor use and the long-term risk of renal failure in diabetes. Kidney Int. 2006;69(5):913-919.
21) Mann JF, Schmieder RE, McQueen M; et al, ONTARGET investigators. Renal outcomes with telmisartan, ramipril, or both, in people at high vascular risk (the ONTARGET study): a multicentre, randomised, double-blind, controlled trial. Lancet. 2008;372(9638):547-553.
22) Yusuf S, Teo KK, Pogue J; et al, ONTARGET Investigators. Telmisartan, ramipril, or both in patients at high risk for vascular events. N Engl J Med. 2008;358(15):1547-1559.
23) Onuigbo MAC. Analytical review of the evidence for renoprotection by renin-angiotensin-aldosterone system blockade in chronic kidney disease—a call for caution. Nephron Clin Pract. 2009;113(2):c63-c70.
24) John P. A. Ioannidis. Adverse Events in Randomized Trials: Neglected, Restricted, Distorted, and Silenced. Arch Intern Med. 2009;169(19):1737-1739.
25) Cook RJ, Sackett DL. The number needed to treat: a clinically useful measure of treatment effect. BMJ. 1995 Feb 18;310(6977):452-4. http://www.ncbi.nlm.nih.gov/pmc/articles/PMC2548824/?tool=pubmed
Recommended Articles

McDougall Quick-Start Program: FREE

A Natural Cure for Depression







