Breast Cancer Treatments: Barbaric and Brutal
By John McDougall, MD
My Aunt Margie developed breast cancer when I was in high school in the early 1960s. She was an intelligent, well-educated, and financially well-off person. We were close. Fortunately, Margie was “cured” after her left breast, lymph nodes, and chest muscles were removed during a procedure called a “radical mastectomy.” Just to make sure they “got it all,” a searing course of radiation was administered post breast amputation. Concurrently, she received potent chemotherapy, which happens to be the same concoction of chemicals given to women in 2017, more than half a century later. The following year her right breast suffered the same fate: amputation and radiation. Well-meaning physicians tortured her in a multitude of manners until her miserable death from metastatic disease three years later, at age 53.
The second time this disease, and the brutal treatments that followed, devastated our family was when 20 years ago my sister-in-law was diagnosed at age 28. She believed in her physicians and accepted every established (and some non-conventional) treatment available. She did not want to discuss her diet with me, unfortunately. Four years later, she died, leaving her husband and two pre-school-age children. Although a small matter in terms of the overall impact, her “state-of-the-art medical care” left her family financially bankrupt. They all lived in my parents’ basement for the next year.
As a physician, I have had the opportunity to counsel hundreds of women with breast cancer. Early in my career I recognized that breast cancer is caused by, and the rate of growth is promoted by, the Western diet. I subsequently published the first scientific study on the dietary treatment of breast cancer in 1984.
Is Your Doctor Breaking the Law?
In 1982, living in Hawaii, I became the sole physician supporting the third “informed consent law” passed in the US. Informed consent is based on the idea that every adult of sound mind has a right to determine what shall be done with his or her own body. This means physicians are required to tell a woman about her options and offer her the meaningful information that she needs to consent to medical procedures, such as breast surgery, radiation, hormone therapy, and chemotherapy. As of 2008, 22 states have enacted informed consent legislation requiring physicians to inform their patients regarding breast cancer treatment consequences and options available. My observation over the past 35 years has been that almost all physicians involved in breast cancer treatment are breaking the laws in these 22 states. Typically, women give me a history of being only offered (and sometimes bullied into accepting) their physicians’ preferred methods of treatment, without any realistic discussion of the consequences, and no alternatives are offered.
The male-dominated medical business seems unstoppable with respect to changing their professional behavior toward women, regardless of more than a half-century of conclusive, consistent scientific evidence, incriminating, beyond argument, their misdeeds. To summarize, so that you can have some control over your future: You must save yourself by becoming well-informed; do not depend exclusively on those in the medical businesses to make your choices.
Natural History Condemns Surgery and/or Radiation
The argument for early detection and aggressive treatment of breast cancer rests on the belief that this disease can be discovered in its early stages, before it has spread to other parts of the body. In the minds of patients, and many physicians, the process looks something like this:
Step 1: A cancer manifests and starts to grow slowly in the tissue (in this case, the breast).
Step 2: With time, the cancer grows into a larger tumor.
Step 3: Eventually, the cancer spreads to the lymph nodes.
Step 4: Finally, the cancer spreads from the lymph nodes to the rest of the body.
Unfortunately, this step-by-step progression from a harmless mass to a body full of disease almost never occurs. Rather, cancer spreads to other parts of the body via the bloodstream in the very early stages of its development. The spread of cancer to the lymph nodes actually occurs simultaneously alongside the spread of the cancer through the blood vessels (venous system).
On a positive note, the rate of growth (doubling time) depends on several factors, including diet. You can change your future.
This diagram will illustrate the growth of breast cancer:
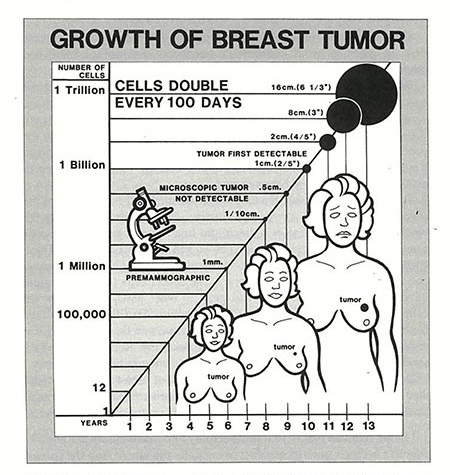
Three-fourths of the time a woman has been a victim of breast cancer has been without her knowledge.73,74 Only during the final stages of this disease is the tumor detectable by any method. Unfortunately, by this time spread to other parts of the body has occurred in almost every case and the disease is incurable.74 Because most of the years of cancer growth are hidden at microscopic levels, efforts toward early detection are unlikely to ever yield much success in saving lives. Our precious health-care dollars would be better spent on efforts toward prevention, such as teaching a low-fat (starch-based) diet.
From McDougall’s Medicine: A Challenging Second Opinion (1985)
Progress Over the Past 3 Decades?
In 1985 my national best-selling book, “McDougall’s Medicine: A Challenging Second Opinion,” provided a comprehensive review of the scientific literature on the treatment of breast cancer. The conclusion: surgery and/or radiation treatments fail to prolong life and cause unnecessary suffering for the patient. All I recommend, for most of my patients, is a lumpectomy with clear margins – no radiation, no lymph node dissection, and no routine chemotherapy. Sometimes I recommend hormone therapy. (Of course, there are particular situations that require other routines.)
This information gathered by me before 1985 could easily be dismissed as outdated. In this newsletter, I will address the medical progress that has been made over the past three decades in the treatment of the disease of the breast itself by surgery and radiation (local treatment). (The treatment of disease spread to other parts of the body, systemic disease, with hormone medications and chemotherapy will be addressed in a future newsletter.)
The Science Behind Surgery
Over the past century, treatment of the tumor discovered in the breast has varied from no surgery at all to removal of both breasts, chest muscles, surrounding lymph nodes, and the arm on the woman’s affected side. Amputation of the breast is called a mastectomy. The modern-day mastectomy operation had its origins in the Renaissance and continued as one standard approach for the next 600 years. Beginning in 1882, the recent “standard for the treatment” of almost all breast cancer has been the Halsted radical mastectomy (complete removal of the breast with its skin, the lymph nodes, and the chest muscles). The operation remained essentially the only option for women for the next 70 years after introduction. In the early 1950s a more conservative approach called the modified radical mastectomy was introduced (the chest muscles were not removed). Radiation has been prescribed for treatment of cancers, treated with and without surgery, since the discovery of x-rays in 1895. A few renegade physicians, notable George Crile from Cleveland Clinic, performed lumpectomies only on selected women. He performed his final radical mastectomy in 1954, and instead became one of history’s pioneers and strongest advocates of conservative breast cancer surgery. Much controversy has been generated concerning “how much treatment of the breast area is necessary in order to live longer?” Properly done scientific studies have provided clear answers.
The first randomized controlled trial comparing treatments, published in The New England Journal of Medicine in 1989, titled “Eight-year results of a randomized clinical trial comparing total mastectomy and lumpectomy with or without irradiation in the treatment of breast cancer,” showed no survival benefits regardless of the aggressiveness of surgery. They found that there was no significant difference in the rates of distant-disease-free survival among the women who underwent lumpectomy (with or without irradiation), despite the greater incidence of recurrence of tumor in the ipsilateral (same) breast in those who received no radiation. A 25-year follow-up confirmed these conclusions.
Note that the addition of radiation after a lumpectomy did not improve survival. However, radiation did prevent local recurrence in the affected breast at a price of significant side effects and financial costs. Following this practice changing research, mastectomies plummeted from the 1988 rate of 77%, to a rate of 35.6% in 2005. They were replaced largely by more conservative surgery (lumpectomy for example) followed by a course of radiation. However, even though no additional research has been published showing benefits of living longer with more aggressive treatment, mastectomy rates began to rise back to 38.4% of surgically treated patients in 2008. The rate of women undergoing mastectomies increased 36 percent between 2005 and 2013, including a more than tripling of double mastectomies.
Efforts to help women by removing all of the lymph nodes in their armpits by surgery and/or aggressive treatment with radiation specifically designed to sterilize even more areas of surrounding lymph nodes have failed to prolong women’s lives.
The total costs for mastectomy vs. lumpectomy plus radiation are similar: $15,000 to $60,000 (US). Like all other businesses, much competition exists in medicine. This competition is reflected in the high variation in “the flavor of the day” accepted as the best treatment and are not justified with new “groundbreaking research” favoring longer survival from a particular regime.
Does Radiation Improve Survival?
The reasoning behind radiation after complete removal of the obvious cancer is to sterilize the remaining breast in order to reduce the risk of local recurrence and future spread of cancer to other parts of the body, ultimately prolonging useful life. Studies look at outcomes such as (1) recurrence of the cancer in the breast, (2) recurrence of the cancer in other parts of the body, (3) risk of dying from breast cancer, and (4) risk from dying from any cause (overall mortality). The most important information the patient wants to know is: “How long am I going to live after various treatments, and which, if any, will cause me to live longer?” The end-point of reduced “breast cancer mortality” only means you did not die from breast cancer. However, you may have died from other causes, many of which were from the treatments given. Therefore, overall mortality is the most important number and the one I report to you in this newsletter. Since the publication of my book, McDougall’s Medicine, two studies and a meta-analysis have been published with the hope that radiation adds meaningful days of living for many women.
Study 1: In 1997 the New England Journal of Medicine published an article, “Adjuvant Radiotherapy and Chemotherapy in Node-Positive Premenopausal Women with Breast Cancer,” where 318 women were divided into two groups treated by two methods. When reviewed 15-years after treatment, there was no significant overall survival benefits from the addition of radiation. However, after 20 years a small improvement in overall survival was found (About 12 fewer deaths with radiation added).
Study 2: In a large follow up of 1708 patients, 10 years after treatment, “Postoperative radiotherapy in high-risk premenopausal women with breast cancer who receive adjuvant chemotherapy. Danish Breast Cancer Cooperative Group 82b Trial,” there was also a small survival benefit with radiation: Eleven fewer deaths were found with the addition of radiotherapy (45 vs 54).
The Meta-analysis: In 2014 the Lancet published a meta-analysis review of 10,801 treated with and without additional radiotherapy, titled the “Effect of radiotherapy after breast-conserving surgery on 10-year recurrence and 15-year breast cancer death: meta-analysis of individual patient data for 10 801 women in 17 randomized trials,” found no significant reduction in overall risk of death gained by the addition of radiation. Mortality without recurrence from non-breast-cancer causes was slightly higher in women allocated to radiotherapy than in women allocated to breast-conserving. Radiation treatment, in addition to killing cancer cells, also damages the heart and the immune system, increasing deaths from non-breast cancer causes.
Other scientific papers on the evidence from breast cancer treatments since 1985 show no overall survival benefits from addition of radiation. A thorough review published also in the Lancet in 2014, “Effect of radiotherapy after mastectomy and auxillary surgery on 10-year recurrence and 20-year breast cancer mortality: meta-analysis of individual patient data for 8135 women in 22 randomized trials,” found no survival benefits from the addition of radiation.
A large population study found no survival benefits from the addition of radiation.
A recent study of women over the age of 69 found a small reduction in local recurrences with the addition of radiation after lumpectomy but no improvement in survival was found over lumpectomy alone. (Tamoxifen, an anti-estrogen medication, was also part of the women’s treatment in both groups).
McDougall’s Medicine: Less Is More
My general recommendations for the treatment of breast cancer remain the same after 40 years of practice:
- Do not rush into treatment. On average, the cancer has already been present for 10 years. Taking a few weeks or months to become well-informed should result in far better decisions and outcomes.
- Remove all of the obvious tumor in the breast with conservative surgery (a lumpectomy with clear margins).
- Refuse routine investigation of your armpit (axillary) lymph nodes.
- Refuse routine post-op radiation treatments.
- Change your diet. You will live longer and with a much better quality of life.
- Do not get routine follow-up visits after your surgery. Only visit your doctor if, and when, a problem arises, such as another lump. No life is lost by this kind of delay and much unnecessary testing and treating is avoided by staying away from doctors.
Reading my chapter on breast cancer from McDougall’s Medicine: A Challenging Second Opinion (1985) will fill in explanations you may have not completely understood with this update. I will discuss updates on systemic treatments, such as hormone- and chemotherapy, in a future newsletter. For now, know that little has changed for most women since I made my recommendations in 1985.
Recommended Articles

Vitamin D: Values for Normal Are Exaggerated

Lessons from the Past, Directions for the Future: The WWI Starch Solution for Denmark







Join the Conversation!
Have a question, a helpful tip, or a story from your journey? Add it below - your voice matters.