Glycemic Index – Not Ready for Prime Time

This article originally appeared in the July 2006 McDougall Newsletter and has been updated in October 2024.
By John McDougall, MD
“Every time I hear about glycemic index I want to puke,” complains Tiffany, one of my nutritionally-oriented friends. “Then I ask the person who is telling me how bad potatoes are if they even know what glycemic index means. They usually tell me glycemic index means the food is high in sugar.” Sugars actually have a very low glycemic index (GI), and according to the popular practice of judging foods based solely on GI, you would be making healthier choices by eating chocolate cake, instead of carrots—or cheese-topped pizza, rather than potatoes. Candies and ice cream, because of their high simple sugar and fat content, are absorbed from the gut into the body slowly; therefore these widely acknowledged “junk foods” have lower GI values than so-believed “health-foods,” like whole grain breads and brown rice.
| Low GI Doesn’t Necessarily Equate with Healthy1 | |
| Junk Foods with GI less than 40 | Healthy Foods with GI greater than 80 |
| Chocolate Cake (38) | Nabisco Shredded Wheat (83) |
| Nestle Quick Strawberry Drink (35 | Corn Meal Porridge (109) |
| No Bake Egg Custard (35) | Jasmine Rice (109) |
| Sara Lee Premium Ice Cream (37) | Brown Rice—Calrose (87) |
| Chocolate Milk with Sugar (34) | Corn Thins (87) |
| M&Ms with peanuts (33) | Baked Potato (85) |
| Pizza Supreme (30) | Boiled Potato (101) |
| Egg Fettuccine (32) | Parsnips (97) |
| Fructose—a pure sugar (19) | Carrots (92) |
The concept of glycemic index was introduced by David Jenkins of the University of Toronto in1981, and the vegetarian diets he and his fellow researchers used consisted of starches, vegetables, and fruits that are low on GI scale, not the many “junk foods” that also have a low GI.2 (Please note that one of the principal researchers from this University of Toronto group, Cyril Kendall PhD, will be a speaker at our next Advanced Study Weekend, Sept. 29 to Oct. 1, 2006).
In the category of “healthy carbohydrates”: fruits, non-starchy vegetables, nuts, and legumes tend to have a low GI. The GI of grains is variable, but typically high. Potatoes and bananas (compared to other fruits) naturally have a higher GI.
What Does GI Measure?
Glycemic index (GI) measures the rise in blood sugar in a person over the two to three hours following the consumption of an amount of food that contains 50 grams of carbohydrate. This rise is then compared to a standard reference: the rise in blood sugar caused by consuming glucose (a sugar) or white bread; also containing 50 grams of carbohydrate. The final result, the GI, is expressed as a percentage. Meat, poultry, fish, cheese, and eggs do not have GI values themselves, because they contain little or no carbohydrate.
In order to make the GI more relevant to daily eating, the concept of “glycemic load” was introduced. Glycemic load figures in the actual amount of food consumed by multiplying the GI of that food times the carbohydrate content of a typical-sized serving of the food. (Example: GI of a baked potato = 85, times 30 grams of carbohydrate in a serving, equals a glycemic load of 26.)
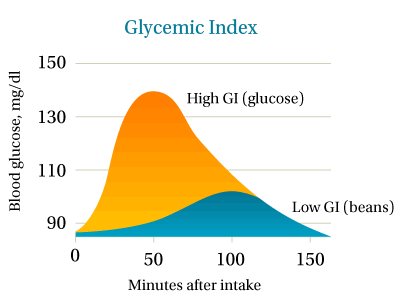
GI Overturns Nutrition Dogma
The findings from the GI demonstrate the falsity of the popular notion that the rates of absorption are a matter of “simple carbohydrates” versus “complex carbohydrates.” The gut is not a passive sieve that allows molecules to pass based on their size—rather it is an active membrane with an “intelligence” that purposefully allows selected nutrients to enter at the correct rate and in the correct amount. The large numbers of carbohydrates found in our foods have a wide variety of chemical compositions and physical structures—as a result of complex interactions, they are digested and absorbed by the human small intestine into the body at different rates—giving rise to diverse blood sugar and insulin responses.
GI Is Just One More Descriptive Quality of a Food
Foods are most often described based on their macronutrient content: like low-carbohydrate, high-fat, high-protein, and low-fiber. The total calories in a serving of a food and cholesterol content are also important descriptives. Some of the micronutrients, such as minerals (sodium, potassium, calcium, etc.), and vitamins (B, C, E, etc.) are considered important enough to be verbally attached to a food, like calcium and milk, and iron and meat.
Foods are also described based upon how they function. The “satiety index” describes the effect of a food on the appetite. For example, potatoes are found to be twice as satisfying as meat or cheese.3 You want your foods to be satisfying. The rise in insulin in the blood after a meal is measured as an “insulin score.” In this case, beef produces more insulin than whole wheat pasta, and cheese more than porridge.4 Insulin drives fat into fat cells, so having a “high insulin score” could be a disadvantage for a person trying to lose weight.
Low GI Diets Can Be Serious Health Hazards
Low GI does not necessarily equate to healthy food choices. The GI of fructose is 19—about the lowest GI you can find. Table sugar (also known as white sugar and sucrose) is half fructose (the other sugar in this disaccharide is glucose). About 55% of the sugar in high fructose corn syrup (HFCS) is fructose. A diet full of sugar is one with a moderate GI. Every year people living in the USA consume, on average, 42.2 pounds of HFCS (GI=60) and 45.2 pounds of table sugar (GI=68). In other words, every day they eat about one-quarter pound of moderate GI food (these two kinds of sugars); which also translates into 500 “empty calories” consumed. “Empty calories” in a food means no essential nutrients, like protein, essential fat, vitamins, minerals, or dietary fiber, are present. Simple sugars, like white sugar and high fructose corn syrup, adversely affect the action of insulin and cause weight gain and elevate triglycerides—all three factors increasing the risk of diabetes. HFCS is believed to be a major player in the rising epidemic of obesity in Western societies.5
Focusing on a low glycemic index diet, while ignoring the other qualities of a food, is also hazardous because the easiest way to decrease the blood sugar response (the GI) to dietary carbohydrate is to consume more protein and fat—the predominant ingredients in meat, poultry, eggs, and cheese. As you know well, these foods are well established to damage your arteries, bones, and kidneys—leading to heart attacks, strokes, osteoporosis, kidney stones, kidney failure, and cancer.
GI Can Be an Impractical Tool
Many people stake their whole health future on the GI. However, from the practical viewpoint of daily use, GI is too complex and changeable to precisely guide a person to the correct food choices. Different studies find widely varying GI values; for example, sweet corn has been found to have a GI of 37, 46, 48, 59, 60, and 62.1 Cooking and cooling changes the food’s GI. The ripeness of the food increases the GI. Disrupting a food’s dietary fiber by grinding, and also removing the fiber, make carbohydrates more easily absorbed, increasing the GI. Mixing foods together results in a GI of the meal that cannot be predicted from the GI of the individual foods. Therefore, even with great effort you will likely be way off your target GI.
High GI and Obesity
Over the past two decades, consumption of foods with high glycemic index values have been associated with various chronic diseases, including type-2 diabetes, coronary heart disease, obesity, and cancer. However, the data are far from clear and consistent—as a result, the usefulness of the GI for the treatment of diabetes and obesity is debated. Some organizations like the Canadian Diabetic Association, consider this tool useful, while the American Diabetic Association dismisses the value of GI in treating diabetes.6
Neither high nor low GI carbohydrates results in excess calorie consumption or weight gain. In fact, a high-carbohydrate diet is crucial in preventing weight gain in those with a tendency for obesity.7,8 Carbohydrate consumption promotes satisfaction of the appetite and higher GI foods do this even better than low GI foods—because the elevation of the blood sugar after eating is one of the key mechanisms in satisfying the appetite and reducing food intake.9 Worldwide, populations of hundreds of millions of people who eat high GI potatoes (Peruvians) and rice (Asians) are trim and active for a lifetime. Compare this worldwide observation to populations of obese people living in the USA, Australia, and Western Europe who feast daily on low GI sugars, fats, meats, and cheeses.
Fat, Not Sugar, Causes Diabetes
According to a statement by the American Diabetes Association, “…there is little evidence that total carbohydrate is associated with the development of type 2 diabetes. Rather, a stronger association has been observed between total fat and saturated fat and type 2 diabetes.”10 Multiple studies have shown an inverse relationship between the amount of carbohydrate consumed and the development of diabetes.11 Populations of people worldwide who eat diets centered on high glycemic index carbohydrates, like rice for rural Asians, and potatoes for people in Peru, are essentially free of diabetes.13,14
Position statement of the American Diabetic Association14
“In subjects with type 2 diabetes, studies of 2–12 weeks duration comparing low glycemic index and high glycemic index diets report no consistent improvements in HbA1c, fructosamine, or insulin levels. The effects on lipids from low glycemic index diets compared with high glycemic index diets are mixed.”
The reasons why carbohydrates benefit diabetics have their roots in our fundamental metabolism. As far back as 1936 Harold Percival Himsworth reported that the ability of insulin to lower blood sugar was improved by eating carbohydrates.15 In contrast, fats in the diet paralyze the activity of insulin, cause insulin resistance, and cause the blood sugars to rise.11 All these changes, combined with the resulting obesity from eating fatty foods, encourage the development of type-2 diabetes. For people now following the Western diet, a change to a low-fat, high-carbohydrate diet slows progression to diabetes.16,17 This same diet will cure type-2 diabetes.18-20
You Should Be a Seeker of Healthy High GI Foods
The primary purpose of eating is to replenish energy—this is most efficiently accomplished thorough the assimilation of carbohydrates—high GI starches and vegetables do this most rapidly. Carbohydrates from our foods pour into our bloodstream to become blood sugars. The brain, nervous system, red blood cells, and kidney cells use only sugar for fuel (under duress the brain can burn fat). Twenty percent of the body’s daily calorie intake goes to the brain, which means a lot of carbohydrate must appear in the bloodstream after eating for this organ to perform efficiently. This is one reason low-carbohydrate diets, such as the one recommended by Atkins, are associated with problems of brain function.21
“Carbohydrate loading” is a technique of eating which is employed by all winning endurance athletes. Carbohydrates, stored as glycogen in the muscles and liver and later released into the bloodstream, provide immediate energy for the whole body during a race. For the most efficient means of replenishing spent glycogen reserves, athletes have learned to choose foods that have a high GI.22,23 Selecting foods with a high GI is just as sound advice for anyone yearning to be strong and energetic throughout the day—not just for athletes.
Little Attention Should Be Given to the GI
Glycemic index is just another way to describe a functional affect of foods on the body. Many popular diets, in particular those which promote high protein, high fat—meat and dairy—eating have placed the GI above all else in their plans to help you lose weight. To ignore the overall qualities of food is unwise. The high GI carbohydrates found in foods like a potatoes or carrots do not make them any more unhealthful than do the simple sugars found in fruits make them unhealthful.
Nutrition-savvy people already know the general concept that legumes, whole grains, fruits and vegetables are good foods. In the whole scheme of the nutritional needs of people the importance of the rate of absorption of carbohydrates (the GI) is overrated and frequently leads the poorly-informed consumer to make bad food choices.
References:
1) Foster-Powell K, Holt SH, Brand-Miller JC. International table of glycemic index and glycemic load values: 2002. Am J Clin Nutr. 2002 Jul;76(1):5-56.
2) Jenkins DJ, Wolever TM, Taylor RH, Barker H, Fielden H, Baldwin JM, Bowling AC, Newman HC, Jenkins AL, Goff DV. Glycemic index of foods: a physiological basis for carbohydrate exchange. Am J Clin Nutr. 1981 Mar;34(3):362-6.
3) Holt SH, Miller JC, Petocz P, Farmakalidis E. A satiety index of common foods. Eur J Clin Nutr. 1995 Sep;49(9):675-90.
4) Holt SH, Miller JC, Petocz P. An insulin index of foods: the insulin demand generated by 1000-kJ portions of common foods. Am J Clin Nutr. 1997 Nov;66(5):1264-76.
5) Bray GA, Nielsen SJ, Popkin BM. Consumption of high-fructose corn syrup in beverages may play a role in the epidemic of obesity. Am J Clin Nutr. 2004 Apr;79(4):537-43.
6) Sievenpiper JL, Vuksan V. Glycemic index in the treatment of diabetes: the debate continues. J Am Coll Nutr. 2004 Feb;23(1):1-4.
7) Jequier E, Bray GA. Low-fat diets are preferred. Am J Med. 2002 Dec 30;113 Suppl 9B:41S-46S.
8) Saris WH. Glycemic carbohydrate and body weight regulation. Nutr Rev. 2003 May;61(5 Pt 2):S10-6.
9) Anderson GH, Woodend D. Effect of glycemic carbohydrates on short-term satiety and food intake. Nutr Rev. 2003 May;61(5 Pt 2):S17-26.
10) Sheard NF, Clark NG, Brand-Miller JC, Franz MJ, Pi-Sunyer FX, Mayer-Davis E,
Kulkarni K, Geil P.Dietary carbohydrate (amount and type) in the prevention and management of diabetes: a statement by the american diabetes association. Diabetes Care. 2004 Sep;27(9):2266-71.
11) Bessesen DH. The role of carbohydrates in insulin resistance. J Nutr. 2001 Oct;131(10):2782S-2786S.
12) Kitagawa T. Increased incidence of non-insulin dependent diabetes mellitus among Japanese schoolchildren correlates with an increased intake of animal protein and fat. Clin Pediatr (Phila). 1998 Feb;37(2):111-5.
13) Llanos G. Diabetes in the Americas. Bull Pan Am Health Organ. 1994 Dec;28(4):285-301.
14) American Diabetes Association. Evidence-based nutrition principles and recommendations for the treatment and prevention of diabetes and related complications. Diabetes Care. 2002 Jan;25(1):202-12.
15) Himsworth HP. Diabetes mellitus: its differentiation into insulin-sensitive and insulin-insensitive types. Lancet 1936;i:127-130).
16) Kim SH, Lee SJ, Kang ES, Kang S, Hur KY, Lee HJ, Ahn CW, Cha BS, Yoo JS, Lee HC. Effects of lifestyle modification on metabolic parameters and carotid intima-media thickness in patients with type 2 diabetes mellitus. Metabolism. 2006 Aug;55(8):1053-9.
17) Kulkarni K. Diets do not fail: the success of medical nutrition therapy in patients with diabetes. Endocr Pract. 2006 Jan-Feb;12 Suppl 1:121-3.
18) Kiehm TG, Anderson JW, Ward K. Beneficial effects of a high carbohydrate, high fiber diet on hyperglycemic diabetic men. Am J Clin Nutr. 1976 Aug;29(8):895-9.
19) Jenkins DJ, Kendall CW, Marchie A, Jenkins AL, Augustin LS, Ludwig DS, Barnard ND, Anderson JW. Type 2 diabetes and the vegetarian diet. Am J Clin Nutr. 2003 Sep;78(3 Suppl):610S-616S.
20) Nicholson AS, Sklar M, Barnard ND, Gore S, Sullivan R, Browning S. Toward improved management of NIDDM: A randomized, controlled, pilot intervention using a lowfat, vegetarian diet. Prev Med. 1999 Aug;29(2):87-91.
21) Wing RR. Cognitive effects of ketogenic weight-reducing diets. Int J Obes Relat Metab Disord. 1995 Nov;19(11):811-6.
22) Hawley JA. Effect of meal frequency and timing on physical performance. Br J Nutr. 1997 Apr;77 Suppl 1:S91-103.
23) Walton P. Glycaemic index and optimal performance. Sports Med. 1997 Mar;23(3):164-72.
Recommended Articles

Three Essential Keys To a Healthy Diet
Cholesterol When and How to Treat It






Join the Conversation!
Have a question, a helpful tip, or a story from your journey? Add it below - your voice matters.