Common Health Problems: Constipation, Hemorrhoids, Varicose Veins
Most people regard a problem with this part of the body as something shameful, something to be hidden: they rarely talk openly about pain and discomfort caused by distresses in the lower bowel. In spite of this secrecy, more kinds of painful sufferings are located in this eight foot segment of writhing tubing than emanate from any other part of the body. Some of the problems are merely nuisances, while others are life threatening, but the one thing that can be said for certain is that none of them need be tolerated as a “normal part of life”.
Constipation means different things to different people. I have met people who tell me that they move their bowels only once in every six to twelve days, and then only with the help of a strong laxative, and they accept this pattern as normal because they know nothing else. Would you accept this as “normal” bowel function, if you had experienced only this sequence since childhood?
Bowel activity associated with good health does vary considerably among “normal people”. For some a movement once every two days may be normal, and others may have three or more stools a day and be in perfect health. The criterion I use for deciding what is normal is that the stool should be moderately soft and easy to pass without pain or strain. The accumulation of feces between movements should not reach the point where severe bloating of the intestine and discomfort occur.
Constipation happens when the stool is hard, small (or “pelletized”, so to speak) and requires physical effort before it is passed. Under such demands, the abdominal muscles must contract, a deep breath must be held as the diaphragm is forced downward. This creates strong internal abdominal pressures to help force the contents out of the colon. This additional force from straining is necessary because the pressure from the contraction of the colon walls is inadequate to evacuate the compacted fecal mass.
One unmistakable sign of this physical effort is that the muscles of the neck and face tense up as you strain to evacuate. If you could see it, you’d notice that your face turns red too. But most people don’t realize that permanent and destructive changes result from these powerful muscle forces, even if they don’t persist for very long.
Veins in your legs are damaged by the straining created by the muscular activity needed for a difficult bowel movement. Valves are located at frequent intervals along the course of the leg veins; they help the blood to rise to the heart, in a stepladder fashion, against the forces of gravity. These valves are stretched and damaged by the high pressures that are required to move small hard dry stools. The valves soon become incapable of holding up the blood. Without valves in good working order, a four foot column of blood presses on the lower veins all day long. One result of this unrelieved pressure is varicose veins, the tortuous blue “worms” which detract so much from the appearance of a person’s legs, often causing pain, and, sometimes ulcers.
Similar to varicose veins in causation if not location are hemorrhoids. All kinds of myths are associated with these painful nuisances. Probably you have heard people say they got theirs from sitting on cold toilet seats, or from having babies.
The veins that become hemorrhoids are located in the very last parts of the intestinal tract, called the rectum and the anus. These veins at this terminus of the gut perform the important function of making a tight seal there, by means of blood-filled cushions to prevent feces and gas from leaking out of the intestine. The seal is actually a double one, and consists of two rows of veins. The higher row at the end of the rectum is called the internal hemorrhoidal veins, and the lower row, those in the anus are covered by skin and are called external hemorrhoidal veins. Underlying these veins is a powerful muscle which acts as the primary regulator in the passage of feces, and is therefore of great social, as well as physical, importance.
The hemorrhoid veins in the rectum suffer a fate similar to the veins in the legs. After years of straining at stool, when each time veins are filled beyond their normal capacity, stretching them like over-inflated balloons, they become permanently dilated and hang out of the rectum. Now they are persistent and painful bulges, with the further troublesome symptoms of bleeding and itching. This same straining causes the anal muscles to be pushed outward. Eventually they become displaced from their normal internal position, and contribute this painful part to hemorrhoidal problems.
Pregnancy can increase hemorrhoidal complications, since the uterus may lie on the veins in the pelvis and cause hemorrhoids to be enlarged. However, this temporary situation does not cause the permanent anal ruination that results from chronic constipation. The best example of the overwhelming influence of a starch based diet in preventing anal problems, even in pregnancy, is presented by African women, who often have as many as 10 babies and yet remain free of troublesome hemorrhoids throughout life. These women never have to strain at stool, because of their diet of grains, beans, and vegetables. (They do not have varicose veins troubles, either.)
Yet another potentially serious problem can be caused by constipation. The natural opening in the diaphragm, through which the esophagus passes, stretches as the stomach is pushed up against it while a person strains to move the bowels. Eventually a tear in the muscular diaphragm happens, and the stomach sits forever above the diaphragm, part way up into the chest in the condition that is called a hiatal hernia.
Constipation is not a consequence of an emotional disorder, at least not initially. However, a lifetime of bowel problems could make anyone question his sanity, and lose his stability. If you eat mostly fiber-free foods, such as animal products (e.g. fish, pork, beef, chicken, lobster, cheese, milk, etc.), visible fats (e.g. butter and corn oil), alcohol, and grains that are highly refined (e.g. white bread and white rice), then little will be left to make feces with adequate bulk. Your BM will resemble hard rabbit pellets.
Fibers are the prime requirement for healthy bowel function. Plant foods contain fibers, a variety of non-digestible complex carbohydrates. After all the soluble components derived from digested fats, proteins, and carbohydrates, along with the vitamins and minerals are absorbed from the small intestine, then non-digestible fibers remain (along with a huge number of friendly microorganisms) to form the bulk of the remnant stool. These fibers have the capacity to hold water, thereby increasing the stool volume further. Also, the more foods and beverages that are consumed, the greater will be the intestinal content, and therefore the frequency and amount of the bowel movement.
A starch-based diet along with vegetables and fruits is a sure cure for constipation. Certain foods, like fruits, contain generous amounts of water and fibers, and therefore contribute to a bulkier, softer stool. Prunes are famous for their beneficial effect on constipation, due to the helpful changes they promote in the lower bowel. Grains contain many kinds of fibers, two of which – cellulose and hemicellulose – are very water absorbent. African natives living on a grain based diet have, on the average, have three large, unformed bowel movements a day. So might you too, with a healthier vegetarian diet.
Avoiding proteins from milk and milk products is very important. I have seen some people who have made nearly a complete change to a health supporting diet. But they couldn’t give up the little bit of skimmed milk in the morning on their dry cereal–and their bowels didn’t work very well. A little dairy protein can literally jam up the works for most people who are sensitive to it.
People who have had intestinal troubles for years, and are labeled as laxative abusers, may have stretched out their colons to twice the normal length and have developed redundant coils of bowel tubing that sort of loop back and forth in the abdominal cavity like a roller coaster. These people need a little extra help. First of all, the colon of a chronic laxative user is accustomed to receiving from a drug the message to contract. The colon has not recently responded to the body’s natural message to contract that should be provided by the stretching of the colon wall as the segment fills with remnants of yesterday’s meals. A person with such a laxative dependency must be encouraged first to renounce his laxatives, and then to wait patiently while the elongated colon fills enough to provide the natural stimulation to evacuate. Initially several days may be needed to fill a very large, stretched out colon; but eventually the muscles in the bowel wall will contract as they should and a movement will follow. Once a natural cycle of filling and emptying is started with high fiber foods, the process continues unaided by anything except the correct choices of foods.
Recommendations
+-A starch-based diet, frequent meals, a little extra water (10 glasses per day instead of the usual 4 or 5) and fruits. Prunes should be eaten as the next step, and following this, for extra help, add flax seeds and bran. Add two to four tablespoons of flax seeds to each cup of a grain, such as rice, before cooking.
As a last resort, I will recommend a non-absorbable sugar, called lactulose (Chronulac, Granulac), this draws water into the colon and helps to end constipation in even the toughest cases. Lactulose is available only with a doctor’s prescription.
References
+-Council on Scientific Affairs. Dietary fiber and health. JAMA 262:542, 1989
Dwyer, J. Health aspects of vegetarian diets (review). Am J Clin Nutr 48(3 suppl):712, 1988
Dehn, T. Hemorrhoids and defecatory habits (letter). Lancet 1:54, 1989
Read, N. Hemorrhoids, constipation, and hypertensive anal cushions (letter) Lancet 1:610, 1989
Burkitt, D. Dietary fiber and disease. JAMA 229:1068, 1974
Burkitt, D. Varicose veins, deep vein thrombosis, and hemorrhoids: epidemiology and suggested aetiology. Br Med J 2:556, 1972
Recommended Articles
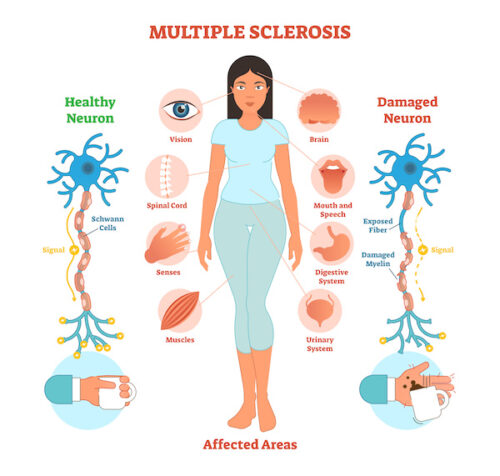
Common Health Problems: Multiple Sclerosis (MS) & Diet

18 Ways to Prevent and Reverse Heart Disease






Join the Conversation!
Have a question, a helpful tip, or a story from your journey? Add it below - your voice matters.